I remember sitting in my car after my first attempt at getting help and thinking, That was it?
Everyone around me kept saying treatment would change everything. Life would turn around. Things would suddenly make sense again.
But when it was over, the quiet truth was this: I still felt like the same person carrying the same weight.
A lot of veterans walk away from treatment with that same feeling. Not because they didn’t try. Not because they didn’t care.
But because the experience didn’t reach the parts of their story that actually needed attention.
If you’ve ever thought I already tried that and it didn’t work, it’s worth knowing something most people don’t say out loud.
Sometimes the issue isn’t the effort.
Sometimes it’s that the approach never matched the life you’ve lived.
If you’re exploring a new path, you might start by learning how a specialized veterans program approaches recovery differently.
When Treatment Focuses on Behavior but Misses the Root
Many treatment environments begin with the same goal: stop the behavior.
Stop drinking.
Stop using.
Follow the schedule.
Attend the groups.
And those things matter. Structure helps people stabilize.
But for veterans, the story often runs deeper than behavior.
Combat exposure, long-term stress, and the emotional shutdown required in high-risk environments can shape the way the brain processes memory, danger, and trust.
When treatment focuses only on surface-level change, it can feel like someone tried to fix the symptoms without understanding the source.
You may leave thinking:
- “I guess I didn’t try hard enough.”
- “Maybe treatment just isn’t for me.”
- “Other people seem to get it. Why didn’t I?”
The truth is, many veterans carry experiences that require a different kind of recovery environment—one that acknowledges trauma, identity, and the psychological impact of service.
The Hidden Layer: How Military Training Shapes Coping
Military culture builds resilience in ways most civilians never experience.
You’re trained to keep moving even when you’re exhausted.
You learn to suppress fear to complete the mission.
You push emotions aside because hesitation can cost lives.
Those traits are strengths during service.
But when someone returns home, those same habits can quietly create challenges.
Emotional shutdown can turn into isolation.
Constant alertness can become anxiety or insomnia.
Unprocessed memories can surface in unexpected ways.
Some veterans describe it as feeling like their nervous system never fully powered down after deployment.
Substances sometimes become the quickest way to quiet the noise.
That doesn’t mean someone lacks discipline or willpower.
Often, it means their brain has been stuck in survival mode for years.
Why Peer Understanding Changes Everything
There’s a moment that happens sometimes in the right recovery environment.
Someone shares a memory about deployment.
They mention something small—a sound, a place, a moment.
And instead of confusion, the room nods.
No one asks you to explain the entire context.
No one looks uncomfortable.
No one changes the subject.
That kind of understanding matters more than most people realize.
For many veterans, healing starts when they don’t feel like they have to translate their experiences to be understood.
Peer connection creates a level of trust that traditional settings sometimes struggle to build.
And trust is what allows people to actually talk about the things they’ve been carrying.
Why Holistic Recovery Matters for Trauma
When people hear the word holistic, they sometimes imagine something soft or vague.
But holistic recovery is really about working with the whole nervous system.
Trauma isn’t just a memory stored in the mind. It’s often stored in the body.
Heart rate.
Muscle tension.
Sleep patterns.
Stress responses.
Holistic approaches address these patterns through multiple channels:
- Movement and physical activity
- Mindfulness or grounding practices
- Outdoor experiences
- Creative expression
- Peer connection and community
These methods help calm the nervous system enough for deeper processing to happen.
When the body begins to feel safe again, the brain can start sorting through memories that were previously overwhelming.
In other words, holistic recovery isn’t about replacing traditional therapy.
It’s about giving the brain more ways to heal.
The Weight Veterans Often Carry in Silence
One thing many veterans share privately is a feeling that they should already have things under control.
Military culture emphasizes strength and self-reliance.
So when struggles appear later—substance use, depression, anger—it can feel like a personal failure.
But the reality is far more complicated.
Veterans may be carrying:
- Survivor’s guilt
- Loss of identity after leaving service
- Disconnection from civilian life
- Memories that never had space to be processed
Those experiences don’t disappear simply because someone leaves the military.
Recovery often involves learning how to live with those memories in a healthier way.
Not by erasing them, but by integrating them into a life that still has purpose.
What Trying Again Really Means
Trying treatment again can feel discouraging.
Many veterans think:
“I already gave it a shot. Why would this be any different?”
But recovery isn’t always a single attempt.
Sometimes the first experience shows what didn’t work.
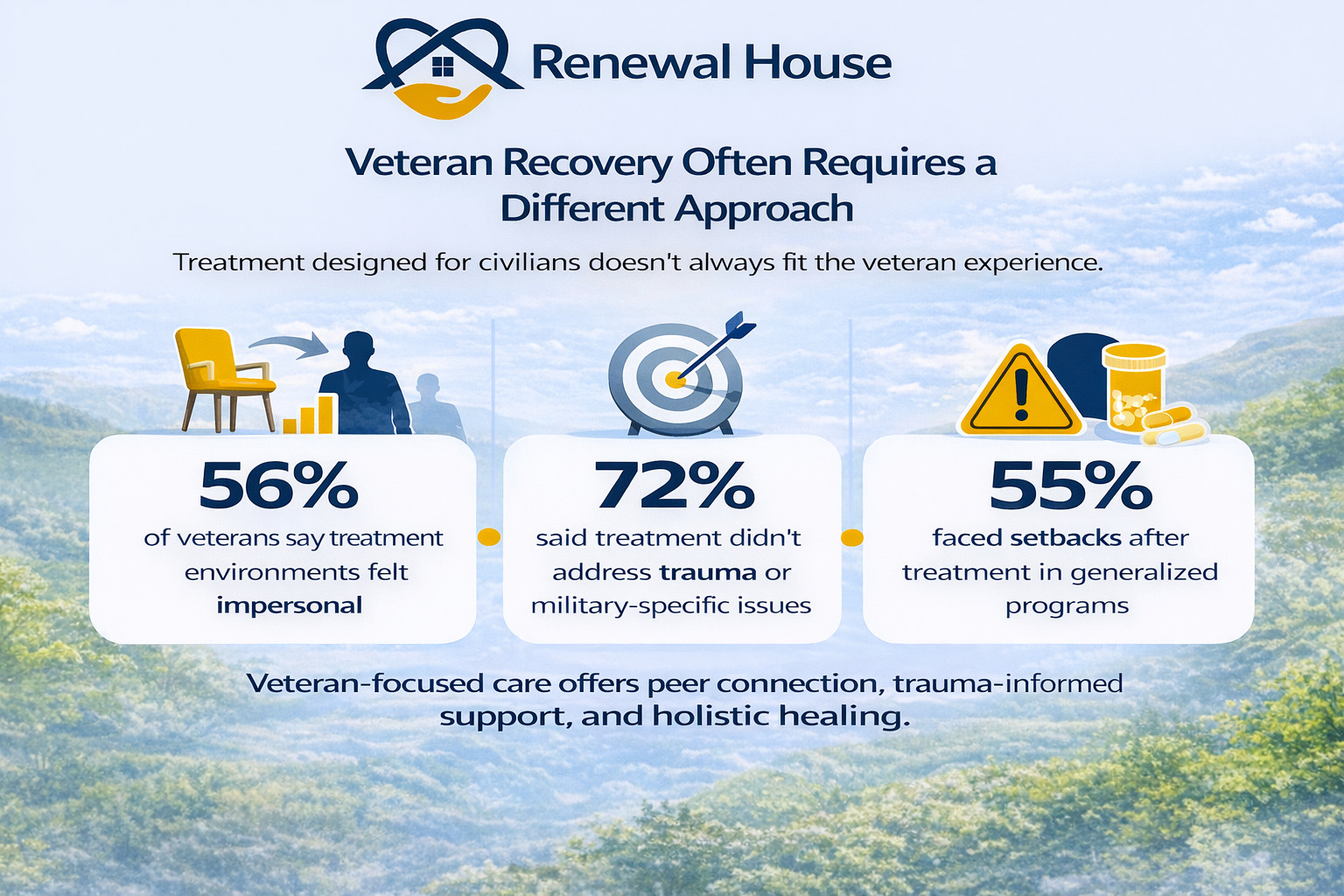
Maybe the environment felt impersonal.
Maybe the group didn’t understand military culture.
Maybe the program focused on rules instead of healing.
Those experiences can actually guide someone toward a better fit.
The right setting often includes:
- Staff familiar with military experiences
- Peer support from other veterans
- Trauma-informed approaches
- Opportunities for holistic healing alongside traditional therapy
When those pieces come together, the process can feel very different.
Not easy—but possible.
A Different Perspective on Recovery
Recovery isn’t about erasing the past.
It’s about building a future where the past doesn’t control every decision.
For veterans, that might mean rediscovering parts of themselves that existed before service.
It might mean finding purpose in helping others.
Or simply learning how to live a quieter, more stable life without constant internal tension.
The path doesn’t look the same for everyone.
But many veterans discover that the right environment—one built around understanding and whole-person recovery—changes the experience entirely.
Frequently Asked Questions
Why do some veterans feel like treatment didn’t work the first time?
Many veterans enter treatment environments that aren’t specifically designed around military experiences. Without trauma-informed approaches or peer understanding, it can feel like important parts of their story are overlooked.
This can lead people to believe treatment itself failed, when the reality is the setting may not have matched their needs.
What makes recovery programs for veterans different?
Veteran-focused environments often include peers who share military backgrounds, which can reduce isolation and increase trust.
These programs also tend to incorporate trauma-informed care and holistic recovery strategies that address both mental and physical stress responses connected to service experiences.
Is holistic recovery effective for veterans?
Holistic recovery approaches can be particularly helpful for people who have experienced trauma.
Practices that regulate the nervous system—such as movement, mindfulness, or outdoor activities—can help veterans process stress and memories in ways that complement traditional therapy.
What if I tried treatment before and relapsed?
Relapse or setbacks are more common than many people realize.
Recovery often involves learning what environments, supports, and strategies work best for you. Trying a different setting—especially one designed for veterans—can sometimes make a meaningful difference.
How do I know if I should consider another recovery option?
If you still feel stuck, overwhelmed, or disconnected despite previous treatment attempts, it may be worth exploring new approaches.
Different environments offer different types of support, and finding the right fit can significantly change the recovery experience.
You Don’t Have to Figure This Out Alone
If you’re a veteran who tried treatment before and walked away thinking it didn’t help, that story isn’t finished.
A different environment—one built around military experience and whole-person recovery—can create a very different path forward.
Call 304-601-2279 or visit our veterans program services to learn more about options available.
If you’re looking for local support, you can also explore care in Charleston or find support in the Eastern Panhandle of West Virginia.
Sometimes recovery doesn’t start with trying harder.
Sometimes it starts with finding people who truly understand where you’ve been.